- Is Vagus Nerve Stimulation Safe? A Nurse’s Guide to Device Safety - April 28, 2026
Given that Vagus nerve stimulation (VNS) devices send electrical signals to a nerve in the brain, it makes sense why people might ask: “Is this safe?”
But VNS refers to techniques that activate the vagus nerve, a key part of the parasympathetic nervous system. That system helps regulate stress, heart rate, digestion, and recovery.
Through my nursing training, supported by a background in psychology and health research, I know that it can be scary to try something that involves electrical pulses. However, Vagus Nerve Stimulation (VNS) has a well-established safety profile in clinical use when applied according to proper guidelines.
Many modern devices are for at-home use, are non-invasive, and applied to areas such as the ear or neck, aiming to support a calmer, more regulated state. Because of this, VNS is increasingly discussed in relation to improving stress resilience, sleep, and post-exercise recovery.
Contents
What Does the Vagus Nerve Do?
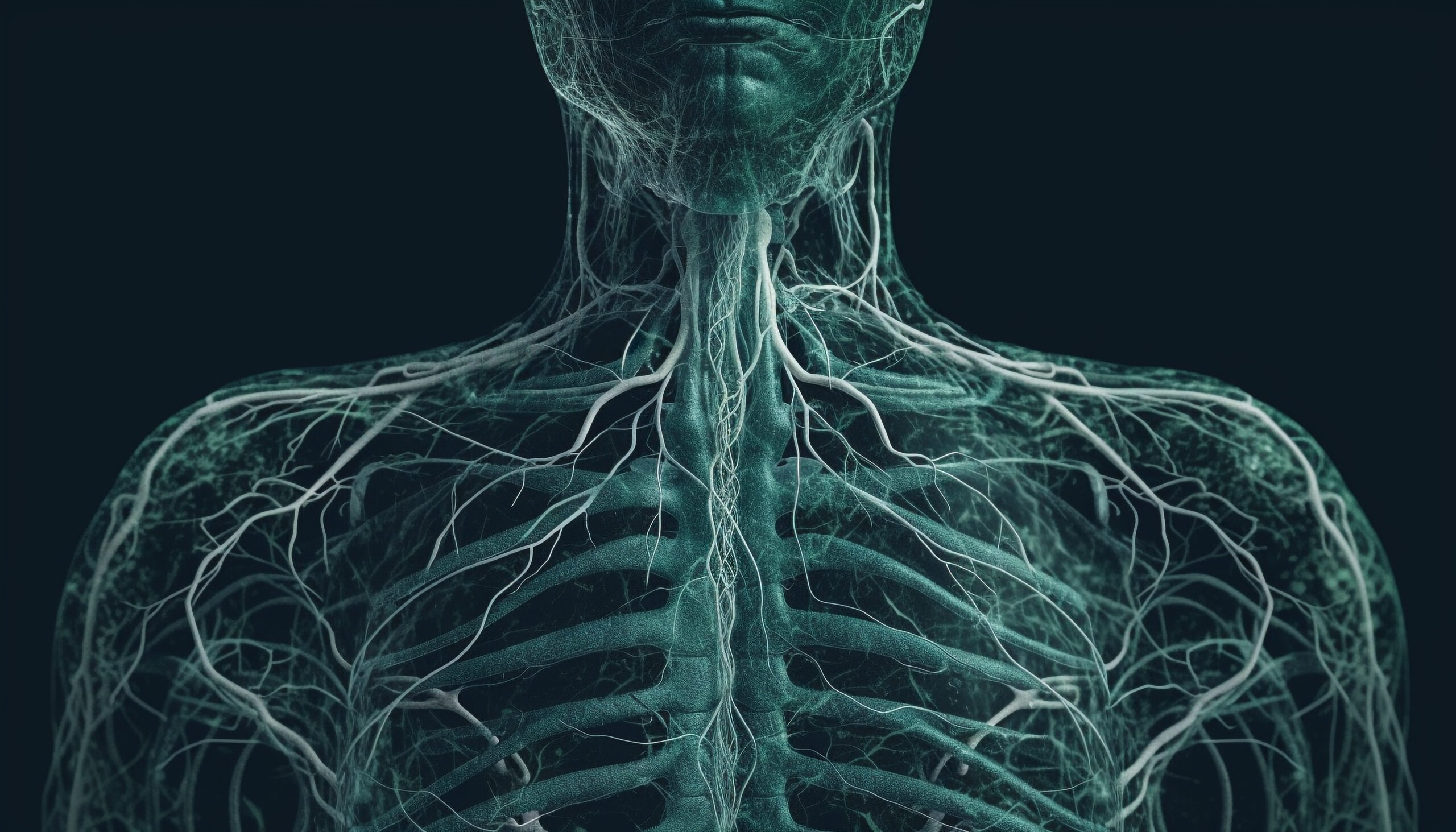
In simple terms, the vagus nerve helps manage the balance between feeling switched “on” and “off.”
The vagus nerve runs from your brainstem down through your chest and into your abdomen, connecting your brain to your heart, lungs, and digestive system along the way. Its main job is running the parasympathetic side of your nervous system, which is the system responsible for rest, digestion, and recovery.
When your vagus nerve is functioning well, your body moves better between those two states. When it isn’t, you can get stuck on the stress side longer than you should, which is where a lot of chronic tension, sleep problems, and digestive issues tend to come from.
Heart rate variability (HRV) is one of the main ways researchers measure vagal activity, and a higher HRV generally reflects a more adaptable, regulated nervous system.
While HRV provides insight into autonomic function, stimulating the vagus nerve doesn’t automatically push that number up or guarantee any specific result. What it does is target the same system that HRV measures, which is why researchers keep coming back to auricular VNS as something worth studying more seriously.
How Non-Invasive VNS Works
There are two main ways to stimulate the vagus nerve without surgery: cervical stimulation and auricular stimulation.
Auricular VNS

Auricular VNS just means stimulating the vagus nerve through your ear – which is the only place on the body where a branch of the vagus nerve comes close enough to the skin to be stimulated externally. That makes it the best access point for VNS.
An ear-based device will clip onto the tragus (that little nub of cartilage at the front of your ear canal) and deliver a mild electrical pulse to the branch of the vagus nerve that runs just beneath the skin there.
That’s it. No needles, no surgery, nothing that goes inside your body.
Cervical VNS
Cervical VNS means stimulating the vagus nerve through your neck.
A device is held or worn against the side of your throat and delivers a mild electrical pulse to the vagus nerve where it runs through that area.
It’s the same basic idea as auricular, just a different access point, and one that some people find less comfortable to wear during normal daily activity. Mostly because, in the neck, the vagus nerve sits deeper beneath more layers of muscle and tissue.
That’s why, while both at-home options are non-invasive, most people consider ear stimulation as the more practical of the two for everyday use. You can clip it on, go about your evening, and take it off 30 minutes later. That ease of use is a big part of why ear-based devices have picked up more traction outside of clinical settings.
What the Research Says About Safety
Non-invasive VNS has a pretty clean safety record so far, and the side effects people actually experience tend to be mild.
A 2018 study looked specifically at how well people tolerate non-invasive VNS, and the findings were reassuring. Most side effects were minor and temporary: things like a tingling sensation where the device touches the skin, minor irritation, an occasional headache, or brief dizziness. Serious reactions were rare and weren’t clearly linked to the stimulation itself.
A 2020 research review echoed this, finding that non-invasive approaches have a good safety record overall. The main note of caution wasn’t about safety. It was about the fact that studies are still conducted inconsistently, which makes it harder to draw firm conclusions across all the research.
On the HRV side, a 2023 analysis found that ear-based stimulation may produce measurable changes in how the heart and vagus nerve are communicating, but results varied enough across studies that researchers are still working to understand when and why it works.
Right now, research suggests non-invasive VNS is safe for most people when used as intended. How reliably it delivers benefits, and how significant those benefits are, is still being figured out.
How to Place These Devices Properly
Getting the placement right for sessions of stimulation is very important when evaluating both safety and the user experience. Here are some tips:
With neck-based devices, you press or hold something against the side of your throat throughout the session. The vagus nerve is accessible there, but some people find it uncomfortable, occasionally noticing throat sensations or temporary voice changes during use.
Ear-based devices let you clip the device onto your tragus, find a comfortable intensity level, and leave it there for your session (usually around 30 minutes). The tragus is where the auricular branch of the vagus nerve sits closest to the skin, which is why it’s the standard placement in clinical research. It’s also why stimulation can be effective at relatively low intensity. Most people barely notice it after the first few sessions.
How VNS Devices Compare
The VNS device market has grown fast enough that it can be genuinely hard to know what you’re actually comparing. Here’s an honest breakdown of the main options, what they do, and where the research actually sits for each.
But remember: not all of these devices work the same way and results will vary.
Neck-Based Electrical Devices (Cervical tVNS)



These sit against your throat and send electrical pulses to the vagus nerve, where it runs through the neck.
GammaCore is a handheld device used to treat acute migraines and cluster headaches. It requires a prescription and is considered more of a clinical tool than a consumer product.
Truvaga is made by the same parent company (electroCore) and includes short sessions of use (around two minutes). However, it requires you to actively hold it against your neck for the entire session duration.
Pulsetto is a lower-cost entry point in neck-based stimulation. However, its data is reportedly pulled from its own funded studies rather than independent, peer-reviewed journals. Pulsetto sessions can last around ten minutes, depending on the program, and it requires a conductivity gel to work.
Ear-Based Electrical Devices (Auricular tVNS)

While there are a few ear-based devices out there, Nuropod is one of the most frequently cited in the peer-reviewed clinical literature on non-invasive VNS. Developed by Parasm, its proprietary AVNT™ waveform technology has been used across more than 50 clinical studies.
The device you would buy from them uses the same technology as those studies, not a consumer adaptation. The European version (Nurosym) is CE certified for neuromodulation, while in the US, Nuropod is currently labeled as a wellness device.
Sessions run around 30 minutes (no gel needed), the intensity is adjustable, and the device clips onto the ear without requiring you to hold it in place. Its clip-on wearability suggests that it might be better as a daily-use device, leading to regular use over time. This might improve overall wellness more efficiently than with occasional sessions.
When to Use a VNS Device

In my nurse training, usability is an essential yet an often overlooked aspect of safety. Health interventions that are comfortable, intuitive, and easy to integrate into daily life are more likely to be adopted and sustained over time.
Many individuals choose to use auricular VNS devices during moments of rest, such as while reading, meditating, or unwinding after exercise. Because these devices can be incorporated seamlessly into existing routines, they offer a practical way to support overall well-being without disrupting daily activities.
Although non-invasive VNS is generally well-tolerated, certain individuals should seek medical advice before initiating use, including those who:
- Have a pacemaker or other implanted electronic device
- Have significant cardiac conditions or arrhythmias
- Have undergone surgery involving the vagus nerve
- Are pregnant
So, Is Vagus Nerve Stimulation Really Safe?
For most people, non-invasive ear-based VNS appears safe and well-tolerated based on current evidence.
It’s not a replacement for medical care, and it works best as one layer in a broader approach to treating sleep issues, stress management, and whatever else you’re attempting to solve.
For people who’ve tried the basics and are still looking for something that addresses their nervous system more directly, it’s good to know there is plenty of research out there to reference – and still more to discover.
When people are equipped with clear, balanced, and evidence-based information, they are empowered to make confident and informed decisions about their well-being.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional before starting any new health intervention, particularly if you have underlying medical conditions or use implanted medical devices.
Sources:
- Cardiovascular Effects Of Auricular Stimulation: A Systematic Review And Meta-Analysis Of Randomized Controlled Clinical Trials (2023)
- International Consensus Based Review and Recommendations for Minimum Reporting Standards in Research on Transcutaneous Vagus Nerve Stimulation (2020)
Safety And Tolerability Of Transcutaneous Vagus Nerve Stimulation In Humans; A Systematic Review (2018)